System Used:
Newton 7.0

In Vivo Imaging of AntiI-αFR Car-Engineered NK-92 Cells Displaying Potent Cytotoxicity Against αFR-Positive Ovarian Cancer
Download Document
Introduction
Ovarian cancer is the most common and most lethal among gynecologic tumors. Folate receptor alpha (FRα), a tumor-associated antigen Folate Receptor alpha, has been reported to be overexpressed in solid tumors like ovarian cancers. The expression of FRα is considered a marker of tumor aggressiveness. However, it is not expressed in normal tissues or is restricted to the apical surface of polarized epithelial cells. FRα is also thought to facilitate resistance to chemotherapy in ovarian carcinoma patients, with higher tissue FRα expression associated with lower response rate to chemotherapeutic agents. It thus can be used as a biomarker for ovarian cancer. Recent studies have suggested that natural killer (NK) cells may be good chimeric antigen receptor (CAR) drivers because of their favorable innate characteristics in specifically recognizing and killing targeted tumor cells. Presently, several clinical trials have confirmed that treatment with CAR-engineered T cells (CAR-T cells) is effective for various tumors such as leukemia and lymphoma and, therefore, represent a powerful approach for tumor therapy in clinical applications. However, the therapeutic effects of CAR-engineered NK cells targeting αFR in ovarian cancer have not been reported.
Objective
In this study, three generations of anti-αFR CAR were constructed, namely αFR-ζ (first generation), αFR-28ζ (second generation), and αFR-28BBζ (third generation), and were highly expressed on the surface of NK-92 cells by lentivirus gene transfection. The antitumor activity αFRCAR- engineered NK-92 cells was evaluated in vivo and imaged with FUSION FX (Vilber Lourmat, France).
Materials & Methods
Xenograft Model of Ovarian Cancer and Bioluminescence Imaging Because NK-92-αFR-28BBζ cells showed significant antitumor activity in vitro (see publication), its cytotoxicity was evaluated in a mouse xenograft model of ovarian cancer. The xenograft ovarian cancer model was established using 6-week-old to 8-week-old female NOD-Prkdcscid IL2rgtm1/Bcgen mice (B-NDG mice). The mice were inoculated intraperitoneally (IP) with 1×106 SK-OV-3 cells expressing firefly luciferase (fLuc+ SK-OV-3 cells). Two weeks after peritoneal inoculation, the mice bearing well-established SK-OV-3 tumors were randomized into 4 groups to receive treatments with different effector cells or PBS at the indicated doses and time intervals. Bioluminescence imaging of tumor-bearing mice was performed using the FUSION FX (Vilber Lourmat, France). After anesthetizing the mice with 10% chloral hydrate, D-luciferin potassium salt (150 mg/kg) dissolved in PBS was IP injected, and bioluminescence imaging was performed 5 to 10 minutes later. All images were collected and analyzed by Fusion software (Vilber Lourmat).
Results
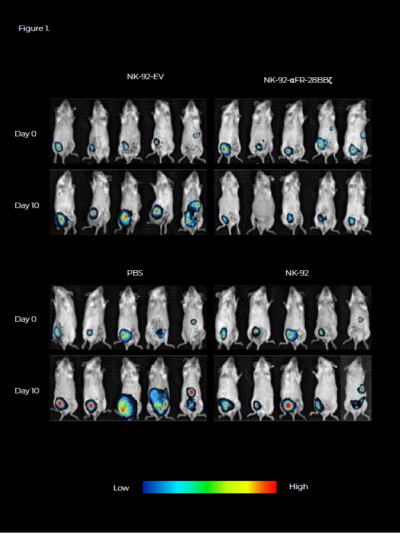
The fLuc+ SK-OV-3 cells were constructed to allow in vivo monitoring of tumor growth by bioluminescence imaging. On day 0, day 4, and day 8, these mice were injected IP with 1×106 NK- 92 cells, NK-92-EV cells, or NK-92-αFR-28BBζ cells. Mice in the control group were IP injected with PBS. Ovarian cancer xenografts in these mice were observed by bioluminescence imaging on day 0 and day 10, as shown in the figure. Mice in the control group, injected with NK-92 cells or NK-92-EV cells, showed significant enhancement in bioluminescence signals in the abdominal cavity on day 10 compared with those on day 0, with the most significant increase observed in the control group (PBS), while the intraperitoneal bioluminescence signals of mice receiving NK-92-αFR-28BBζ cells injection significantly decreased on day 10.
Conclusion
These results suggested that NK-92-αFR-28BBζ cells can effectively eradicate tumor cells, inhibit the development of ovarian cancer in vivo, and thus prolong the survival of the tumor bearing mice. These results enlighten the abilities of the FUSION FX (Vilber Lourmat, France) in imaging therapeutic effects of CAR-engineered NK cells targeting αFR in ovarian cancer.
Learn more about one of the tools that was central to this research
Authors
Xiang Ao,*† Yu Yang,‡ Weiqiang Li,* Yan Tan,*† Wei Guo,*†Luoquan Ao,*† Xiao He,*† Xiaofeng Wu,*† Jianchuan Xia, Xiang Xu,*† and Jianxin Guo‡.(2019)
*State Key Laboratory of Trauma, Burn and Combined Injury, Department of Stem Cell & Regenerative Medicine, Daping Hospital and Research Institute of Surgery; †State Key Laboratory of Trauma, Burn and Combined Injury, First Department, Daping Hospital and Research Institute of Surgery; ‡Department of Gynaecology and Obstetrics, Daping Hospital and Research Institute of Surgery; §Department of Biochemistry and Molecular Biology, College of Basic Medical Sciences, Third Military Medical University, Chongqing; and ∥State Key Laboratory of Oncology in South China, Collaborative Innovation Center for Cancer Medicine, Sun Yat-Sen University Cancer Center, Guangzhou, P.R. China